Interest and knowledge of the gut microbiome exploded in the last decade or two, and for good reason.
The gut is turning out to be more than just a tube that runs from your mouth to your anus.
Although this tube is technically ‘outside’ the body, it’s becoming evident that what happens in the gut, don’t stay in the gut.
Hippocrates said it quite frankly about 2400 years ago. Yet, it’s like after all these years, we didn’t know how profoundly interconnected our guts are with the rest of our bodies.
What Is a Microbiome?
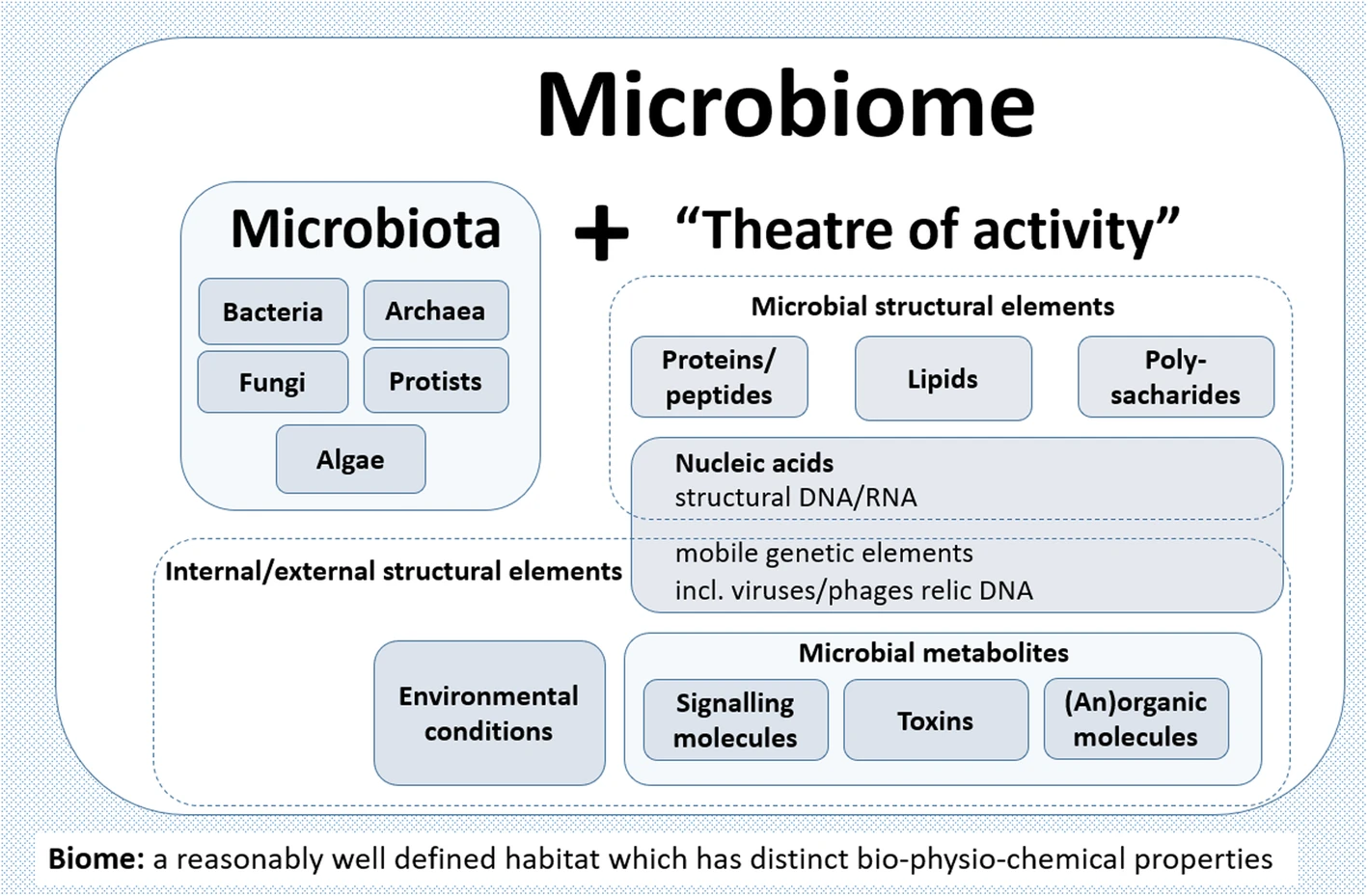
Image Credit: BioMed Central: Microbiome definition re-visited: old concepts and new challenges
“A schematic highlighting the composition of the term microbiome containing both the microbiota (community of microorganisms) and their “theatre of activity” (structural elements, metabolites/signal molecules, and the surrounding environmental conditions)”
Microbiota: The community of microorganisms living in an environment, comprising of for example bacteria, viruses, archaea, algae, fungi and protists.
Microbiome: The microbiota as well as their genes, including the environment and host.
We have a microbiome not only in our guts, but also on our skins & sexual organs, and in our mouths, lungs and noses.
But what is so intriguing about our gut microbiome?
Here are eleven things that charm my interest:
1. You Are More ‘Gut’ Than Human
Our guts host 10 times more bacteria than all the human cells in the entire body, totaling roughly 100 trillion microbes, representing as many as 5,000 different species.
On a genetic level, 3.3 million genes are reported to exist in your gut, compared to just 22,000 genes present in the human genome.
If you thought your genetic make up is what makes you unique, think again.
As humans, we are 99.9% identical to each other in terms of our own genome, whereas the gut microbiome of each individual can be 80-90% different from one another.
A popular ‘fact’ which claims that our gut bacteria weighs 1.5 – 2kg (more than your brain), was however found to be grossly overestimated.
2. Ancient Chinese Medicine Involved Eating Poop Soup
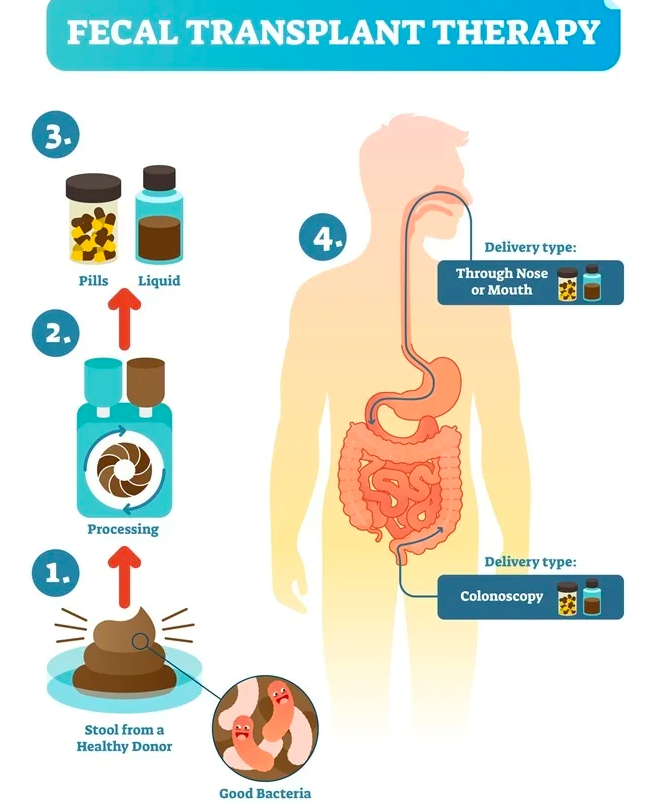
You’ve probably heard of fecal transplants fairly recently, but the first record of using feces as a therapy dates back as far as fourth century China.
Golden / Yellow Soup containing fermented fecal matter from a healthy person (as a primary ingredient), was used to treat diarrhea and food poisoning.
The sick person ate the soup, upon which the bacteria in the ingested stool would inhabit the gut of the sick person and bring about healing.
I wonder if a spoonful of sugar managed to make that medicine go down?
Don’t worry, I won’t share the recipe 😉
The shit did not stop there though…
In the seventeenth century, veterinarians transplanted stool, orally and rectally, to treat animals.
It’s claimed that during WW2, German soldiers ate warm camel stool to treat dysentery. Based on the (beneficial) bacterial composition of camel dung however, this story is possibly not true.
But it was not until 1958 that fecal microbiota transplantation (FMT) was first introduced to mainstream medicine and reportedly used by physicians in US hospitals.
To date, the most successful treatment for patients with antibiotic resistant C. difficile is FMT.
Thankfully, FMT does not involve eating smelly Golden Soup anymore. Colonoscopies, tubes, capsules or enemas are used today.
Since the health of your gut is linked with an array of other conditions, FMT is suggested to be a “possible emerging treatment for a wide range of disorders including Parkinson’s disease, fibromyalgia, myoclonus dystopia, multiple sclerosis, obesity, insulin resistance, metabolic syndrome, and autism” (source).
Both chronic fatigue syndrome and insulin sensitivity in people with metabolic syndrome have indeed demonstrated a positive response to experimental FMT.
3. The Gut Bacteria Have a Range of Different Roles

Out gut bacteria have several important functions, including:
- promoting normal gastrointestinal function
- providing protection from infection
- regulating metabolism
- making up more than 75% of our immune system
- producing energy from the food we eat
- produce neurotransmitters such as glutamate, GABA, serotonin, and dopamine
- helping manufacture enzymes
- synthesis of vitamin K and B vitamins
- playing a role digestion
- regulating hormones like estrogen, thyroid stimulating hormone (TSH), serotonin, and stress hormones
4. Your Gut Microbiome Is Based In Your Intestines (Not Your Stomach)
The gut microbiome is mostly based in our intestines, as the stomach environment is too acidic for the bacteria to survive.
5. That Gut Feeling
Since gut health is so closely related to mental health (see next point), early development and overall illness, I had to add the video and following quote from the ever intriguing Dr. Gabor Maté:
“How many of you had the experience where you had a powerful gut feeling about something, but you didn’t pay attention to it and you were sorry afterwards?
At some point in your childhood you got separated from yourself. There is no infant born without their gut feeling. Infants are totally connected with their gut feelings. Have you ever met a 2-year-old who didn’t know how to express their gut feeling? That means that in this culture, something very powerful happens to alienate to your true self.
Cause the world couldn’t stand to who you really were. And your parents were too stressed themselves to honor and recognize who you really were.
Then we become alienated from ourselves, we shut down our gut feelings and our gut feelings are not luxuries. They tell us what is right and what is wrong. They tell us what is dangerous and what is safe. And they tell us what is true and what is false.
So, when we are alienated from our gut feelings we no longer have a sense of reality or a sense of truth.”
6. Your Gut Is Called Your “Second Brain”
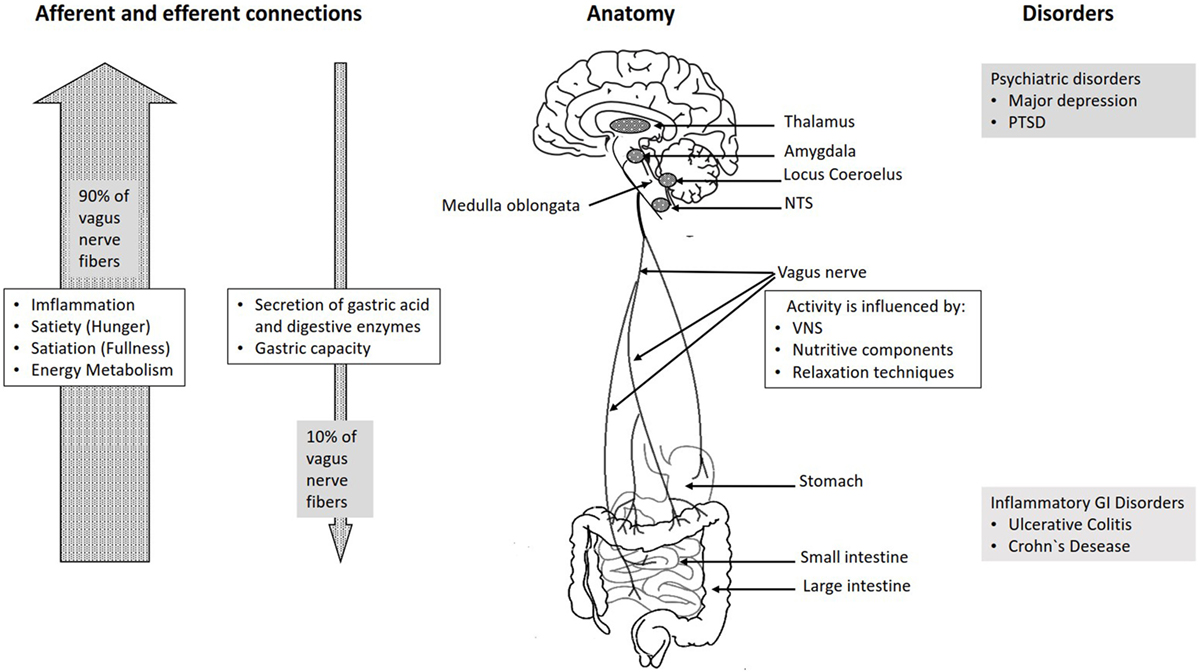
The gut-brain axis (GBA) consists of bidirectional communication between the central and the enteric nervous system, linking emotional and cognitive centers of the brain with peripheral intestinal functions. Recent advances in research have described the importance of gut microbiota in influencing these interactions.
– The gut-brain axis: interactions between enteric microbiota, central and enteric nervous systems
Perhaps not surprising, considering that we get ‘feelings’ in our guts!
Ever been to the toilet at a race, an hour (or less) before the start? If you have, you’ll understand the link between nervousness and toilet runs (pun intended).
Via the vagus nerve, bacteria in our guts are in constant communication with our brains, and vice versa.
This important connection has been termed the ‘gut-brain axis’.
But it’s not only mental stress that affects our guts.
Few realise that a whopping 95% of serotonin, over 50% of dopamine and even some GABA get produced in the gastrointestinal (GI) tract!
They are all neurotransmitters and responsible for (amongst other things) happiness (serotonin), calmness (GABA), and motivation and mood (dopamine).
Your gut bacteria can even contribute to suboptimal neurological performance later in life.
7. A Fury Kiss A Day Keeps The Baddies Away

Image Credit: Africa Studio by Adobe Stock
A general shift away from natural environments with reduced exposure to soil and animals, seems to be detrimental to our gut microbiomes.
It’s been found that children raised in homes with dogs or cats have less risk of allergic diseases.
This happens in a dose dependent fashion – the more pets, the better the effect.
Evidence is demonstrating a link with gut microbiome patterns:
Early exposure to pets increase the abundance of two bacteria which protect against childhood allergies, respiratory viruses and even obesity.
Gotta let your dogs sleep inside!
8. Your Gut Affects Your Weight And Metabolism
Traditional approaches to fight obesity have not shown promise in promoting a decline in obesity prevalence. The gut microbiota are becoming widely appreciated for its role in regulating metabolism and thus represents a target for new therapies to combat obesity and associated co-morbidities.
Overweight and obese individuals are generally found to have gut dysbiosis characterised by a low diversity of gut bacteria.
Dysbiosis “involves the loss of beneficial microbial input or signal and an expansion of pathogenic microbes” (source).
Researchers can tell with 90% accuracy whether you’re overweight or lean, based on looking at your gut microbiome composition alone!
Obesity has actually been induced in mice by transplanting the gut micobiota from obese mice to previously lean mice.
Just look at this fascinating finding from a study:
“Introducing a single bacterium that has been associated with obesity (Enterobacter cloacae) into germ-free mice led to weight gain, a disturbed glucose tolerance, higher systemic lipopolysaccharide binding protein (LBP) concentrations and lower adiponectin levels.”
Calories in, calories out be damned!
If you’ve been on my Gut Reset page, you will also know the story of the lean woman who got a fecal transplant from her obese daughter. And yes, you guessed it – she became obese too.
Diet and exercise were not been able to get her weight back down.
I find it baffling that lifestyle changes was the chosen intervention, since it obviously was not the cause of her weight gain!
If only she would try dealing with the cause by resetting her gut.
In an interesting study (published 11 November 2022) on rhesus macaque monkeys, it was found that grooming behaviour (a good indicator of social connectedness in primates) was positively correlated with better gut health.
Lead author of the study, Dr. Katerina Johnson, said:
“Here we show that more sociable monkeys have a higher abundance of beneficial gut bacteria, and a lower abundance of potentially disease-causing bacteria. It is particularly striking that we find a strong positive relationship between the abundance of the gut microbe Faecalibacterium and how sociable the animals are. Faecalibacterium is well known for its potent anti-inflammatory properties and is associated with good health.”
In a study on humans, it was found that social interactions with relatives and friends were strong predictors of gut microbial diversity.
Microbial diversity is recognized as one of most important signs of good gut health.
10. One Course of Antibiotics May Make Permanent Changes To Your Gut

While antibiotics certainly have saved many lives, it unfortunately gets prescribed and taken willy nilly, far too often.
Doing so is deleterious for overall health, as antibiotics cause a rapid and profound loss of the diversity of the gut flora.
Even after two to four years of taking a single course of antibiotics, some bacterial groups do not recover completely.
Since all bacteria are wiped out by antibiotics, and about 70-80% of our immune cells are located in the gut, our immunity takes a beating each time we take antibiotics.
This can set off a vicious cycle if getting sick, needing more antibiotics, compromising the immune system, which in turn makes us susceptible to getting sick again. And so the cycle prevails.
11. Having Leaky Gut Does Not Necessarily Mean You Have Gut Symptoms

Chris Kresser’s post highlights the fact that skin problems, heart failure, autoimmune conditions, mental illness, obesity, diabetes, allergies, autism spectrum disorder and depression can all be manifestations of having a leaky gut.
When fixing your gut, you therefore inevitably improve overall health.
In fact, the following was noted in a Covid article published in the Critical Reviews in Food Science and Nutrition journal just last week:
“An impaired gut microbiota has been observed in COVID-19 patients, irrespective of the presence of GI symptoms”.
Also:
“Studies have shown that people with long-COVID have reduced commensal bacterial population and altered overall gut microbiota.“
I feel that this last point warrants a full post.
Keep an eye out for it! ?



Wow Thanks for this post i find it hard to identify exceptional information and facts out there when it comes to this subject matter appreciate for the thread site